You've been managing your blood sugar. Taking your medicines. Watching what you eat. But here's something your doctor may not have told you clearly enough — uncontrolled diabetes is quietly threatening your vision, and cataracts may be forming in your eyes right now without you knowing it.
Millions of people with diabetes in India develop cataracts 10 to 15 years earlier than people without diabetes. If you or a loved one is living with diabetes, visiting a trusted eye hospital in lucknow for a comprehensive eye check-up isn't just a good idea — it's urgent. At Abhinav Drishti Hospital, our specialists see this connection between diabetes and early cataracts every single day, and early detection makes all the difference.
Let's break down exactly what's happening inside your eye, why diabetes accelerates cataract formation, and what you can do about it.
What Exactly Is a Cataract?
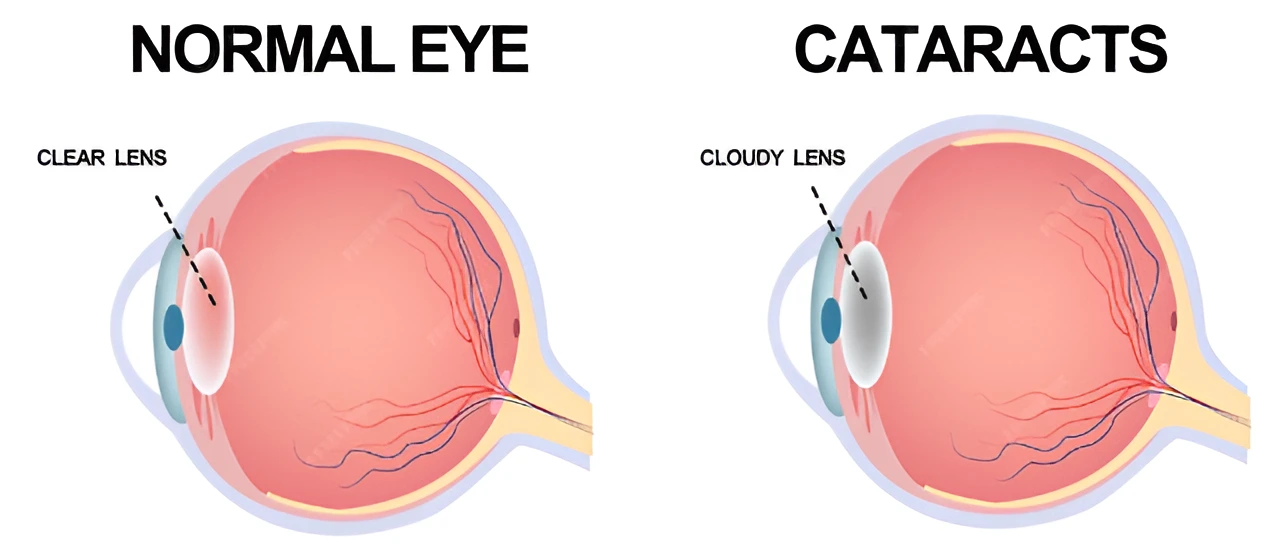
Your eye has a natural lens — a clear, transparent structure sitting just behind your pupil. Its job is to focus light onto the retina so you can see clearly.
A cataract occurs when this lens becomes cloudy or opaque. Light can no longer pass through cleanly. Vision becomes blurry, foggy, or dull — like looking through a dirty windshield that no amount of wiping can clean.
Cataracts are the leading cause of reversible blindness in India. While aging is the most common cause, diabetes accelerates the process dramatically and can cause cataracts at a much younger age.
The Diabetes–Cataract Connection: What Happens Inside Your Eye
This isn't just a statistical association. There is a clear, well-understood biological mechanism linking high blood sugar to lens clouding.
1. The Sorbitol Buildup Problem
When blood glucose levels stay elevated for extended periods, the lens of your eye absorbs excess glucose. Your body then converts this glucose into a sugar alcohol called sorbitol through a process called the polyol pathway.
Here's the problem: sorbitol cannot easily exit the lens. It accumulates and draws water into the lens cells. This swelling disrupts the precise arrangement of lens proteins, causing them to clump together — and those clumps are what we see as cloudiness or opacity. That's a cataract beginning to form.
2. Oxidative Stress Damages Lens Proteins
High blood sugar also generates free radicals — unstable molecules that attack and damage the proteins in your lens. Normally, the lens has its own antioxidant defense system. But in diabetic patients, chronic high glucose overwhelms these defenses.
The result? Lens proteins break down faster than the body can repair them. The lens progressively loses its clarity.
3. Glycation of Lens Proteins
High glucose directly attaches to lens proteins in a process called glycation (the same mechanism behind HbA1c measurements in diabetes blood tests). Glycated proteins lose their flexibility and transparency, contributing further to lens clouding.
How Much Earlier Do Diabetics Get Cataracts?
This is where the numbers become alarming.
| Factor | General Population | People with Diabetes |
|---|---|---|
| Typical Age of Cataract Onset | 60–70 years | 40–50 years |
| Risk of Developing Cataracts | Baseline | 2–5× Higher |
| Rate of Cataract Progression | Gradual (years) | Faster (months to years) |
| Risk of Bilateral Cataracts | Lower | Significantly Higher |
| Surgical Complexity | Standard | Higher (due to other diabetic eye changes) |
Diabetics don't just get cataracts earlier — they often get them in both eyes and they progress more rapidly.
Types of Cataracts More Common in Diabetics
Not all cataracts are the same. Diabetic patients are especially prone to two specific types:
- Posterior Subcapsular Cataract (PSC): This type forms at the back of the lens and is strongly linked to diabetes. It progresses quickly and affects reading vision and glare sensitivity early on.
- Nuclear Cataract: Develops in the central (nuclear) zone of the lens. Common in older diabetic adults and causes progressive blurring of distance vision.
- "Snowflake" Cataract: A rare but distinct diabetic cataract that can develop rapidly in young people with severely uncontrolled Type 1 diabetes. It appears as white, snowflake-like deposits in the lens.
Warning Signs You Should Never Ignore
Diabetic cataracts can be sneaky. Many people assume blurry vision is just a sign that they need stronger glasses. Here are the real warning signs to watch:
- Blurred or hazy vision that doesn't improve with glasses or contact lenses
- Increased sensitivity to glare — headlights at night or bright sunlight during the day
- Fading or yellowing of colors — objects appear dull or washed out
- Frequent changes in your eyeglass prescription
- Double vision in one eye
- Difficulty reading in bright or low light
- A feeling of looking through fog or frosted glass
If you have diabetes and experience any of these symptoms — even mildly — do not wait for your next routine check-up. Get your eyes examined immediately.
Diabetes Also Damages Your Eyes in Other Ways
Cataracts are just one piece of the picture.Diabetes affects the entire eye, making regular eye care essential.
- Diabetic Retinopathy: High blood sugar damages the tiny blood vessels in the retina. This can cause leaking, bleeding, and abnormal vessel growth that may lead to vision loss.
- Diabetic Macular Edema (DME): Fluid leaks into the macula (the center of the retina), causing distorted or blurred central vision.
- Glaucoma: People with diabetes are about twice as likely to develop glaucoma, a condition where eye pressure damages the optic nerve.
- Fluctuating Vision: Rapid changes in blood sugar levels can cause temporary blurriness as the lens shape changes due to fluid shifts.
This is why diabetic eye exams are much more thorough than a routine vision test — every part of the eye needs to be carefully assessed.
Can You Prevent Diabetic Cataracts?
You may not be able to completely prevent cataracts if you have diabetes, but you can significantly slow their development and protect your vision.
- Control Your Blood Sugar: Keeping HbA1c within your target range reduces sorbitol buildup and limits oxidative damage to the lens.
- Manage Blood Pressure and Cholesterol: High blood pressure and cholesterol worsen the damage diabetes causes to eye blood vessels. Managing all three together is essential.
- Quit Smoking: Smoking increases oxidative stress in the body and accelerates cataract formation.
- Wear UV-Protective Sunglasses: Ultraviolet light damages the lens over time. Wearing good-quality UV-blocking sunglasses helps slow this damage.
- Eat a Vision-Protective Diet: Foods rich in antioxidants such as leafy greens, carrots, bell peppers, and citrus fruits help protect the lens. Vitamins C and E, lutein, and zeaxanthin are especially beneficial.
- Get Regular Dilated Eye Exams: Every diabetic patient should undergo a comprehensive dilated eye exam at least once a year, or more frequently if eye disease is already present.
When Is Cataract Surgery Needed for Diabetics?
The decision to surgically remove a cataract is based on how much it is affecting your daily life and vision — not just how it looks on a scan.
For diabetics, surgery is recommended when:
- Vision impairment interferes with driving, reading, or daily activities
- The cataract prevents proper monitoring of the retina (making diabetic retinopathy management harder)
- Vision loss is progressing rapidly
Cataract surgery is one of the safest and most effective surgeries in the world. It typically takes 15–20 minutes, requires no hospital stay, and restores clear vision very effectively.
However, diabetic patients require extra pre-surgical preparation. Blood sugar must be well-controlled before surgery to reduce infection risk and promote healing. The retina must be assessed and any retinopathy treated before cataract removal. Your surgeon needs to plan carefully for the best outcome.
Diabetes is a lifelong condition, but vision loss from diabetic cataracts does not have to be. The relationship between high blood sugar and lens clouding is well understood — and so are the ways to slow it down, detect it early, and treat it effectively.
Don't wait for your vision to get noticeably worse. If you have diabetes, your eyes are at risk right now. An annual eye examination is not optional — it is a non-negotiable part of diabetes management. Book your comprehensive diabetic eye check-up at Abhinav Drishti Hospital today. Our experienced specialists will assess your complete eye health — from lens clarity to retinal health — and create a personalised care plan to protect your vision for years to come.